State of the Art Stroke Interventions by Dr. Vikas Rao
Stroke is the leading cause of disability and the 3rd leading cause of death in the US. Approximately 800,000 Americans a year will suffer a stroke, which is about once every 40 seconds. It’s important to understand these interventions for patients with aneurysms, arteriovenous malformations, brain bleeds, ischemic strokes, and other cerebrovascular disorders.
Ischemic Stroke
The majority (over 85%) of strokes are ischemic – caused by thrombosis or embolic blockage of cerebral vessels. Similar to a heart attack, these strokes can be thought of as a “brain attack”. Many strokes are preventable, however if one does occur it is extremely important to identify it immediately and get the patient to a stroke center where they can be evaluated and treated quickly. While historically stroke was a disease that was somewhat passively managed, we now have new treatments available to open acute brain blockages and reverse the symptoms of stroke.
TPA – Clot Buster Drug effective in Stroke
Since the FDA approved recombinant tissue plasminogen activator (TPA) for use in the treatment of ischemic strokes in 1996, it has remained the gold standard for stroke treatment. TPA can be administered to patients who present to stroke capable hospitals within 3 hours (and in select cases 4.5 hours) of the onset of symptoms provided they do not have a contraindication.
While an excellent first line therapy and effective in many strokes, TPA is often ineffective in occlusions of the larger cerebral vessels – the internal carotid, proximal middle cerebral, or basilar arteries. These large vessel occlusions (LVOs) can result in extremely disabling and sometimes fatal strokes. With recent improvements in technology and the publication of pivotal randomized trials, the treatment paradigm for emergent LVO has changed. Now we can offer emergent endovascular treatment options for LVO that are superior to TPA alone.
Acute Ischemic Stroke Intervention with Stent Retrievers
Early neuro-interventional treatments for stroke relied on corkscrew-like devices to capture a clot or an intracranial microcatheter to aspirate clot after mechanically disrupting it. Unfortunately, these early devices had limited and were not proven to improve outcomes. The newest generation of stroke devices, stent-retrievers, have shown improved results.
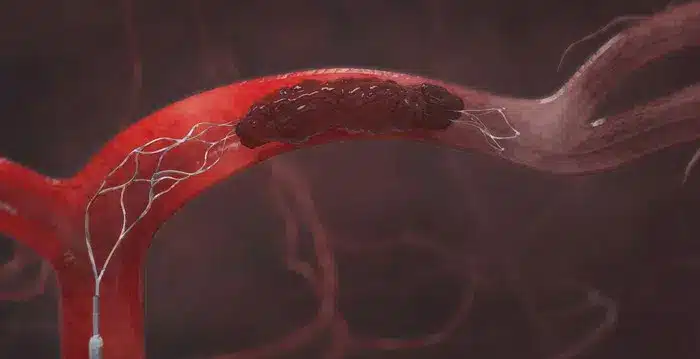
Stent-retrievers are tiny self-expanding mesh tubes that unlike cardiac or carotid stents, are attached to a wire so they can be pulled back after being deployed. They are deployed into intracranial vessels across a thrombus using special microcatheters. Once the stent is deployed it slowly integrates into the clot over a few minutes before it is slowly removed, bringing the clot with it. Special suction catheters are sometimes used to aid in clot removal and prevent distal embolization. These devices have an approximately 85% recanalization rate in large vessel occlusions as opposed to a 30% recanalization rate in the older generation of devices.
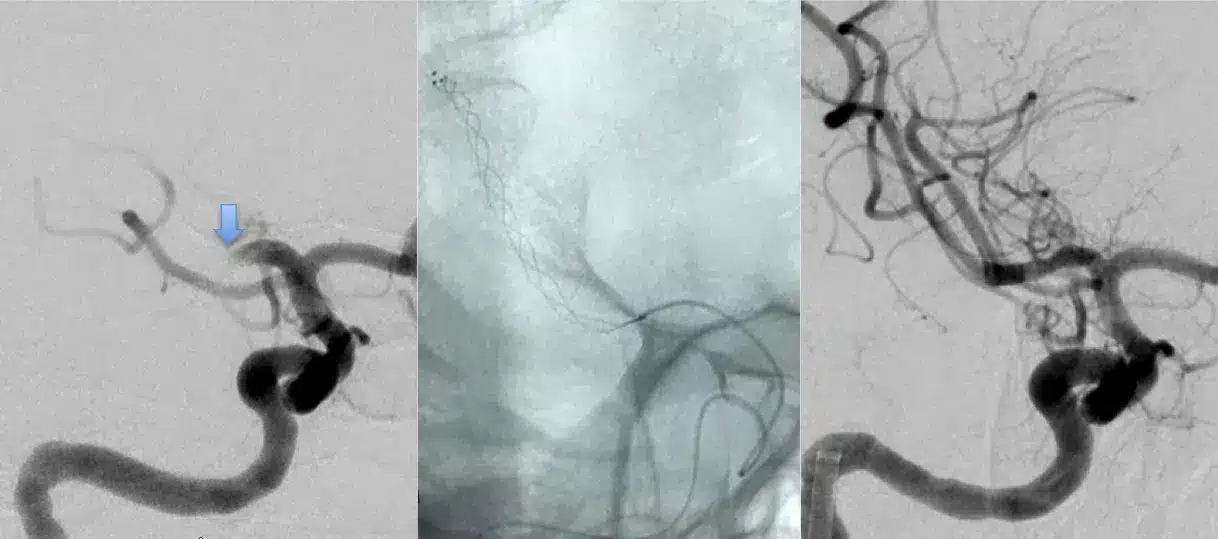
Mechanical thrombectomy is usually performed after administration of TPA, but can be performed for patients who present outside the TPA window as long as there is imaging evidence that the brain downstream of the clot is still salvageable (usually within 6-8 hours). The procedure does carry a risk of peri-procedural strokes, intracranial hemorrhage, renal damage from contrast, and groin complications. When weighed against the outcomes from untreated large vessel strokes, however, the benefits often outweigh the potential risks.
In the January 2015 edition of the New England Journal of Medicine the MR CLEAN randomized control trial was published showing superiority of mechanical thrombectomy with stent-retrievers and TPA vs. TPA alone. 4 additional trials have been published recently which have unanimously shown similar results. A meta-analysis in the March 2016 Jama Neurology looked at over 1200 patients involved in these 5 trials and found almost twice as many patients achieve functional independence at 90 days with the procedure vs. TPA alone.
Emergent intracranial thrombectomy with stent-retrievers has become the standard of care for select patients with LVO. Today, doctors working together in Stroke Teams provide this service and other advanced stroke care to our community.
Welcome to the office of neurosurgeon Dr. Vikas Rao, where your health comes first. Below are some of the neurosurgical treatments that we offer in Mission Viejo, CA:
Contact us today
Your concerns are important to us, and we want to make sure all of your questions are answered so you understand your options. Please contact our office with any questions, and our team will be happy to assist you.
Give us a call
We're open to serve
Our doctor and staff are devoted to our patients. Please fill out the form below with any questions or to schedule an appointment and our team will get back to you within 24 to 48 hours.